Recommended citation: Toumazis, I., Kwon, C., and Batta, R. (2013), "Value-at-Risk and Conditional Value-at-Risk Minimization for Hazardous Materials Routing", in Handbook of OR/MS Models in Hazardous Materials Transportation (Eds.:R. Batta and C. Kwon), Springer
Lung Cancer Screening Strategies
Lung cancer is the number one cancer related cause of death in the United States with more than 158,000 new deaths expected in 2016. This translates to approximately 1 in every 4 cancer related deaths to be attributed to lung cancer. Smoking has been identified as the main cause of lung cancer. Despite recent decline in smoking prevalence, lung cancer is the most common type of cancer affecting both males and females in the United States.
The National Lung Cancer Screening Trial (NLST) demonstrated that screening individuals at high-risk for lung cancer with low-dose computerized tomography (CT) reduces lung cancer mortality rates by 20%. In particular, NLST enrolled individuals between 55-74 years old, with a smoking history of at least 30 pack-years and which were current or former smokers with no more than 15 years since cessation.
Following the findings of the NLST, the United States Preventive Services Task Force (USPSTF) recommended annual screenings using low-dose CT for people that met NLST eligibility criteria. Later on, the USPSTF extended screening up to age 80. More recently, the Centers for Medicare and Medicaid Services (CMS) decided to provide coverage for low-dose CT screening for heavy current and former smokers (as defined by NLST) from age 55 up to age 77.
As part of the Cancer Intervention and Surveillance Modeling Network (CISNET) an NCI-sponsored consortium we aim to estimate the health benefit and harms of different screening strategies.
Colorectal Cancer Chemotherapy Scheduling Problem

Colorectal cancer (CRC) is the third most commonly diagnosed cancer with 136,830 estimated new cases in 2014, and the second most lethal affecting both men and women with 50,310 estimated deaths. The number of fatalities associated with CRC has decreased during the last couple of decades (on average by 2.8% each year), mostly due to increased public awareness and improved screening and treatment methods. Despite such improvements, only about 12.5% of metastatic CRC (mCRC) patients survive longer than 5 years.
In 2009, 143,000 hospitalizations were recorded for CRC patients, which ranks CRC as the forth most frequent type of cancer hospitalization. The total cost from these hospitalizations was $2,598 million with $2,200 mean cost per day and 8.3 days average length of stay. The above statistics emphasize the high cost of mCRC treatment, and the need for the development of cost efficient guidelines.
CRC patients have a number of viable treatment options including surgery, radiation therapy, chemotherapy and targeted therapy. Systemic treatment, such as chemotherapy, is administered to patients diagnosed with late-staged disease; either alone or combined with radiotherapy and/or targeted therapy. Chemotherapy treatment affects both cancer and normal cells. Therefore, oncologists consider the tradeoff between tumor size reduction (death of cancer cells) and toxicity (death of normal cells) resulting from the treatment. In addition, oncologists often encounter tumor drug resistance, which develops after long exposure to the same regimens.
Despite the existence of multiple CRC treatment guidelines, the question of if and when to use which treatment remains controversial. Individualized treatment is an approach that is widely considered to be the most promising and effective. These guidelines, even though they admit that personalized treatment is more effective, do not provide such for all patients, simply because this is not yet feasible. Furthermore, guidelines do not consider the cost of cancer treatment nor the knowledge accumulating from the routine evaluations of the mCRC patients during the treatment period. This research develops individualized chemotherapy treatment schedules based on several patient demographic factors, disease characteristics, and history of treatment.
The overall objective of this project is to improve treatment decision making process for mCRC patients, incorporating the challenges introduced from cost restrictions, toxicity and tumor's drug resistance. Analytical models will be developed to address how existing clinical data can be used to answer the following questions:
Which chemotherapy regimen should be administered given patient's demographics, disease characteristics, and current toxicity levels?
At what time point each chemotherapy drug should be administered given the history of treatment?
For how long each treatment should be given to a patient to avoid tumor resistance?
What is the best treatment choice for each patient under a particular budget?
For the purposes of this study an extensive literature review was conducted. Namely, we collected the reported outcomes from the resulting publications of numerous clinical trials to form a mCRC specific database. We used this database to calibrate our models. A complete list of the puplications used to construct the database is available here .
Hazardous Materials Transportation

Hazardous material (HazMat), as defined by the U.S. Department of Transportation Pipeline and Hazardous Materials Agency, is a substance or material capable of posing an unreasonable risk to health, safety, or property when transported in commerce. There are various types of hazardous material transportation which range from movements of relatively harmless products, like hair spray and perfumes, to massive shipments of gasoline by highway cargo tanks, to transportation of poisonous, explosive, and radioactive materials. Accidents involving transporting HazMats are very rare. However when one does happen, the damages and consequences can be catastrophic in a means of both human casualties and residential environments.
During the year 2013 (as recorded by the Pipeline and Hazardous Materials Safety Administration) there have been 16,033 HazMat incidents which resulted in 165 injuries, 12 deaths and damages of total worth $79,319,578. Note that the procedure of transporting these kinds of materials is divided in four phases: the loading, in transit, in transit storage and unloading. The cost of the damages resulted by incidents during the transit phase had a total cost of $70,663,313 and the injuries during the same phase were 49, among which 11 needed hospitalization. From all 12 deaths that occurred in 2013, 10 of them took place in the process of transit and only two occurred during the other three phases, specifically one in the loading phase and one in the unloading phase.
On average, more than 800,000 shipments occur daily in the U.S. mostly using trucks as mean of transportation especially for relatively short distances. Using trucks for transportation is very popular since they are operationally flexible. In other words, trucks among other transportation modes, have the advantage of pick up and drop off HazMats very close from the origin and to the destination, respectively. However, the number of incidents involving the truck transport mode is the highest. In addition, trucks can be easily used for terrorist attacks against people and buildings. These statistics along with the possible threats emphasize the importance of efficient and effective regulative operation of urban traffic networks involving HazMat transportation.
HazMat accidents rarely happen (low-probability incidents), but if they do occur, then the consequences can be disastrous (high-consequence incidents), reflecting on both the population and the environment. It is important to make a risk-averse route decision in HazMat transportation. In this project, two new risk measures are introduced addressing the problem of safety in HazMat transportation. Namely, Value-at-Risk (VaR) and Conditional Value-at-Risk (CVaR) models are developed and shown to be proper risk measures for flexible HazMat route decision making. Furthermore, challenges arising from data uncertainty are addressed utilizing robust optimization techniques, proposing an additional risk measure called Worst-case Conditional Value-at-Risk (WCVaR).
HazMat Data
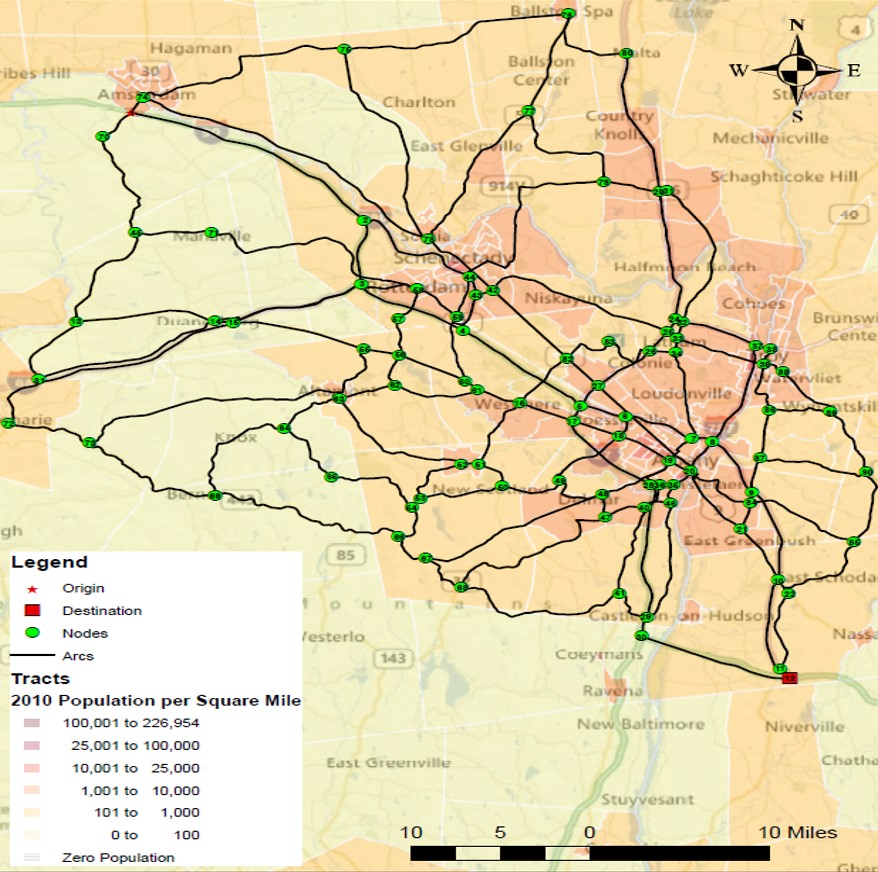
Through the course of this project, two vehicular networks were developed along with their respective data sets. In particular, data were collected for a part of the vehicular road networks of:
HazMat Data Sources
Federal Highway Administration, Publications & Statistics
Federal Motor Carrier Safety Administration, Statistics and Facts
New York State Department of Transportation, Traffic Volume Data
Pipeline and Hazardous Materials Safety Administrator, Data & Statistics
New York State Thruway Authority
Greater Buffalo-Niagara Regional Transportation Council, Transportation Data Management System
U.S. Hazardous Materials Report, Commodity Flow Survey, U.S. Census Bureau
HazMat Incidents
Incident Reports Database Search, U.S. Department of Transportation
Yearly Incident Summary Reports–Hazmat Intelligence Portal, U.S. Department of Transportation
Spills and Accidents Database, The Right-to-Know Network
Databases: Hazardous Material Incident Logbook Search, Arizona Department of Environmental Quality
Environmental Releases, Delaware Department of Natural Resources and Environmental Control
Hazardous Materials Spills, Illinois Emergency Management Agency
Spill Incidents Database Search, New York Department of Environmental Conservation